The tremendous success of modern laser vision correction has helped establish refractive surgery comanagement as a leading subspecialty in optometric eye care during the last two decades. With the establishment of new technologies and the refinement of surgical techniques, we are rapidly approaching a point when patients with nearly all varieties of refractive error will be afforded the opportunity to achieve excellent levels of uncorrected acuity.
 | |
|
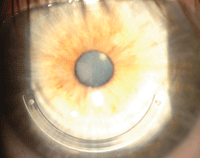
Corneal flap creation procedure with the Intralase (Abbott Medical Optics) femtosecond laser system.
|
Thus, all primary eye care providers should have a working knowledge of the procedures currently available––as well as those on the near horizon––so your patients can make informed decisions about which surgical options are most suitable. Inevitably, patients interested in refractive surgery will have a variety of vital questions. So, how do you most effectively counsel patients in the decision-making process?
Here, we present a stepwise approach that will help you determine the most appropriate procedure for each patient who ask you you about surgical vision correction.
General Refractive and Health Assessment
A thorough evaluation of ocular and general systemic health is key in the initial assessment of any refractive surgery candidate. Also, it is imperative to have a good understanding of the patient’s visual goals and expectations. Early presbyopic low myopes, who hope to eliminate spectacle use altogether, and patients with unrealistic expectations require extensive education about the potential outcomes. Presbyopic or pre-presbyopic patients need to understand the concept of accommodative loss with age. As such, it is best to illustrate what they can expect when performing near visual tasks when fully corrected for distance acuity. Such patients can opt for a monvision outcome with surgery designed to undercorrect the non-dominant eye. Alternatively, they can elect for full correction with the option of presbyopic inlay enhancement surgery.
Those with active or chronic ocular conditions such as glaucoma, dry eye, blepharitis or recurrent herpes simplex keratitis do not qualify for surgery until these issues are under control, have resolved or have been successfully treated.
From a systemic standpoint, patients with active collagen vascular disease (e.g., lupus, rheumatoid arthritis, Sjögren’s syndrome) are not strong candidates for refractive surgery. Neither are cancer patients who are currently undergoing chemotherapy. While these systemic conditions are not absolute contraindications to surgery, affected individuals should only consider surgery if the underlying disease is quiescent.
|
Appropriate Age Range
|
A comprehensive ophthalmic evaluation is imperative, as the results will help tailor your surgical recommendation. Appropriate testing should include a refraction, pachymetry measurement, corneal topography, ocular surface evaluation, binocular vision assessment and peripheral retinal evaluation. A cycloplegic refraction is a necessary last step in the refractive surgical evaluation of a phakic patient.
Thin corneal pachymetry (i.e., readings less than 480µm) or asymmetric topography will require further assessment of corneal structural integrity with technologies such as the Pentacam (Oculus) to ascertain whether laser vision correction remains a viable option. These measurements also will help you determine whether alternative treatments might offer a better safety profile for the patient, with equivalent or even superior visual outcomes.
Once you’ve determined that the individual has good ocular and systemic health, you, the surgeon and the patient can begin deciding upon the most appropriate option.
Laser Vision Correction
When patients ask about long-term vision correction options, it is very likely that most of their questions will center upon LASIK and photorefractive keratectomy (PRK).
When coupled with femtosecond laser flap creation, today’s customized, excimer laser-based corneal ablative procedures yield significantly better safety and predictability profiles than surgeries performed with past technologies. Femtosecond laser-produced corneal flaps are remarkably consistent in shape, placement, size and depth. Flap side cut design with this instrument permits better stability and is associated with a significantly lower incidence of flap slip, flap striae and postoperative dry eye.
Further, wavefront-guided LASIK permits the calculation of customized ablation profiles for those patients with significant higher-order aberrations. Such procedures––specifically tailored to the individual patient’s optical system––improve the likelihood that they will achieve uncorrected vision that’s equal or, in some cases, superior to the results they’ve experienced with contact lenses or glasses.
In conjunction with these surgical advances, we now have enhanced corneal tomography devices that enable us to more accurately predict postoperative outcomes in patients who are good candidates. Such commercially available tomographers include the Pentacam, Galilei G2 (Zeimer) and Visante Omni (Carl Zeiss Meditec). These instruments allow for early detection of corneal float, elevation abnormalities or keratoconic progression, which cannot always be detected with routine corneal topography or keratometry alone.
Approximately 98% of bladeless LASIK and PRK patients who are deemed to be good candidates experience outstanding postoperative visual success.1 Myopia of up to 9.00D, hyperopia up to 2.50D and astigmatism up to 3.50D can be successfully treated via either approach (however, LASIK permits faster, more comfortable visual rehabilitation than PRK).
To minimize the risk of postoperative ectasia, individuals with thin corneas (i.e., less than 480µm) and normal topography are better candidates for PRK than LASIK. For patients with thin corneas and asymmetric/irregular topography or high levels of ametropia, further evaluation with your refractive surgeon will be required to assess surgical management decisions.
High Astigmatism
Individuals who present with myopic astigmatism in excess of 3.50D still may be potential candidates for laser vision correction. following treatment with astigmatic keratotomy using the femtosecond laser. This procedure can correct up to 6.00D of astigmatism, and will permit patients to proceed with laser vision correction after a six-week healing period.2
Likewise, GP contact lens patients who struggle with high astigmatism should consider femtosecond laser astigmatic keratotomy to improve corneal morphology, lens fit and comfort.
Implantable Collamer Lenses
For individuals with myopia equal to or greater than 9.00D, abnormally thin corneas, dry eye or abnormal topography, a phakic IOL may be an excellent refractive option. Patients with less than 9.00D of myopia also may be candidates for phakic IOLs if they prefer a non-laser corrective option.
| Working Alongside Ophthalmology
It is essential to establish a strong relationship with an experienced refractive surgeon to ensure the most successful comanagement experiences. Above all else, choose only to work with a surgeon who will respect you as an equal partner in the decision-making process for your patients. Be mindful of the potential consequences in partnering with a self-proclaimed “pioneer” or an “aggressive marketer,” and remain cautious of working with surgeons whose only tangible credential is “a high volume of refractive procedures performed.” Consistently research refractive surgeons in your area by speaking with both patients and your optometric colleagues. Only choose to work with a surgeon who can provide the full spectrum of available procedures so that patients are not simply “shoehorned” into a procedure that might be familiar to the surgeon, but not necessarily the most appropriate option for the individual. Subspecialty training in cornea is a real plus, as those surgeons are best qualified to address anterior segment issues. Successful refractive surgery generates great satisfaction. And while the majority of patients should enjoy excellent outcomes, it is critical to partner with a surgeon who is well versed on all issues that could potentially arise after even uneventful surgery. When patients ask you about refractive surgery, the discussion will inevitably turn to the question of candidacy. As the field of refractive surgery has grown, a one-size-fits-all approach is no longer appropriate. A patient who may not have been the right candidate for traditional laser vision correction might now benefit from a host of excellent alternatives, including phakic intraocular lens implantation, laser astigmatic keratotomy, intrastromal implants or even femtosecond laser refractive clear lens exchange. |
One such lens, the Visian ICL (Staar Surgical Company), uses a hybrid hydrogel material referred to as a “collamer” that is comprised of collagen and is therefore highly biocompatible.
The lens is implanted into the posterior chamber and positioned behind the iris. Also, both eyes typically are implanted on the same day––creating a “LASIK-like” experience for the patient.
Study data suggests that ICL implantations are both safe and effective. However, one report noted a very small risk of significant anterior subcapsular cataract development in 1% of implanted patients.3 If this should occur, symptomatic patients should be referred for standard cataract surgery.
A toric version of the lens soon will be available for myopes with associated astigmatism. This will allow for the correction of up to 4.00D of astigmatism following ICL implantation. The FDA’s ophthalmic devices panel issued premarket approval status for the Visian Toric ICL in March of 2014.
Other phakic IOLs being developed include the Veriseye (Abbott Medical Optics) and AcrySof Cachet (Alcon). Both are anterior-chamber lenses positioned in front of the iris.
Keratoconus Stabilization
Until fairly recently, patients with keratoconus or pre-keratoconus were not considered candidates for laser vision correction. However, several technological advances have helped make refractive surgery possible for affected individuals. By working in concert with your refractive surgeon, you can customize a plan that not only improves visual quality, but also halts ectasia.
• Corneal collagen crosslinking (CXL) is a revolutionary treatment for patients with keratoconus. In the past, we treated all keratoconic patients with spectacle lenses first, followed by toric soft lenses and then rigid lenses before surgical intervention (i.e., penetrating keratoplasty) was contemplated. Today, however, we believe that CXL should be considered an early, first-line treatment to halt disease progression.
The CXL procedure exposes the cornea to UVA illumination after saturation with 0.1% riboflavin drops. Early keratoconic patients with pachymetry measurements greater than 400µm are the most suitable candidates for treatment.
Although rigid contact lenses may offer acceptable visual results, they do not stop keratonconus progression. CXL, on the other hand, has been shown to slow or halt the progression of corneal ectasia and astigmatic distortions. A 2010 study indicated that 97% of patients who undergo CXL during the early stages of the ectactic process showed no evidence of further disease progression.4
Patients who present with early ectatic signs on the posterior corneal surface may now be considered for combined CXL and lamellar or surface excimer ablation procedure.5 For this procedure, the patient’s cornea is saturated with riboflavin immediately after the refractive treatment, and then is exposed to the UV irradiation process. This increases collagen lamellar and strand crosslinking, enhancing corneal rigidity.
It is worth noting that some refractive surgeons are now
combining CXL with LASIK and PRK (i.e., PRK and LASIK Xtra [Avedro, Inc.]) in non-keratoconous patients to reduce or eliminate the risk of postoperative ectasia.
• Intacs. In patients with more advanced keratoconus, femtosecond-assisted Intacs (Addition Technology) implantation is an effective approach to improve visual function. The laser is capable of creating precision placement channels that accept the intrastromal rings. This measure enhances corneal morphology and allows for better uncorrected acuity, improved spectacle correction and increased contact lens tolerance.
A preoperative evaluation of corneal morphology will determine whether symmetrical or asymmetrical ring placement is advisable. Additionally, we recommend that patients consider combination CXL and Intacts implantation to further decrease the likelihood of keratoconic progression.
• Laser-assisted keratoplasty. For keratoconus patients who present with advanced disease or exhibit significant scarring, corneal transplantation is often the only management option. Fortunately, femtosecond technology offers improved comfort, safety and predictability while speeding visual recovery.
With traditional penetrating keratoplasty, the surgeon removes the diseased host cornea using a circular trephine. However, laser-assisted keratoplasty allows the surgeon to produce a custom-shaped, multiplanar incision to remove the cornea and then create a matching donor graft. With this “jigsaw puzzle” fit, host/donor apposition is now much more accurate. Thus, laser-assisted keratoplasty patients typically experience rapid healing, as well as visual recovery within six weeks of surgery.6 Additionally, patients usually develop very low levels of postoperative regular astigmatism.
Presbyopia Correction
Until very recently, monovision LASIK was the only viable surgical option for presbyopic patients. While the surgical management of presbyopia continues to be challenging today, femtosecond laser refractive clear lens exchange with multifocal or accommodating intraocular lenses is gaining popularity.
 |
|
|
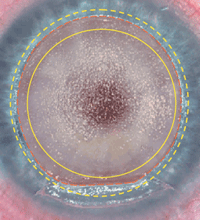
Intacs (Addition Technology) intrastromal ring implantation in a patient with asymmetric keratoconus.
|
Additionally, two new corneal inlay surgical solutions await FDA approval––the AcuFocus Kamra and the ReVision Optics Raindrop.
• The Kamra inlay is designed for implantation into a femtosecond-created pocket that’s centere d over the pupil. This effectively reduces pupillary diameter to 1.5mm, and improves near vision via an optical pinhole effect without significantly impacting distance acuity. Post-LASIK and pseudophakic IOL patients experience significant improvements in near vision function following Kamra implantation.7
• The Raindrop inlay is a hydrogel lens that measures 2mm in diameter. It is positioned under a LASIK flap, which creates a prolate cornea and yields a multifocal effect.
All eye care providers should enhance their working understanding of the latest refractive surgery options available to their patients. This is a field that continues to advance rapidly and, as such, requires ongoing education to most effectively guide patients seeking your advice and counsel.
|
Links to Dr. Fox’s Surgical Videos on YouTube • Femtosceond laser corneal flap creation for LASIK • Astigmatic keratotomy using a femtosecond laser |
Dr. Fox is the medical director at the Clarity TLC Refractive Surgery Center in West Orange, NJ. He may be contacted at: [email protected].
Dr. Quinn is the president of Omni Eye Services of New Jersey.
Neither author has any direct financial interests in any of the products mentioned.
1. Fox ML. Collective review of in-office refractive surgery survey. Data collected from 2009-2014.
2. Fox ML. Femtosecond astigmatic keratotomy before LASIK can be beneficial. Ocular Surgery News. Available at: www.healio.com/ophthalmology/cornea-external-disease/news/print/ocular-surgery-news/%7Bca69d701-eda0-44e4-967e-eac34c350887%7D/femtosecond-astigmatic-keratotomy-before-lasik-can-be-beneficial. Accessed September 10, 2014.
3. Sanders DR. Anterior subcapsular opacities and cataracts 5 years after surgery in the visian implantable collamer lens FDA trial. J Refract Surg. 2008 Jun;24(6):566-70.
4. Caporossi A, Mazzotta C, Baiocchi S, Caporossi T. Long-term results of riboflavin ultraviolet A corneal collagen cross-linking for keratoconus in Italy: The Seina eye cross study. Am J Ophthalmol. 2010 Apr;149(4):585-93.
5. Spoerl E, Huhle M, Seiler T. Introduction of cross-links in corneal tissue. Exp Eye Res. 1998 Jan;66(1):97-103.
6. Fox ML. Ocular Surgery News. Article pending publication, October 2014.
7. Personal communication with Jeff Machat. August 2014.

